 1 Chronic kidney disease (CKD) stimulates release of a fibroblast growth factor, FGF-23, that causes myocardial hypertrophy. 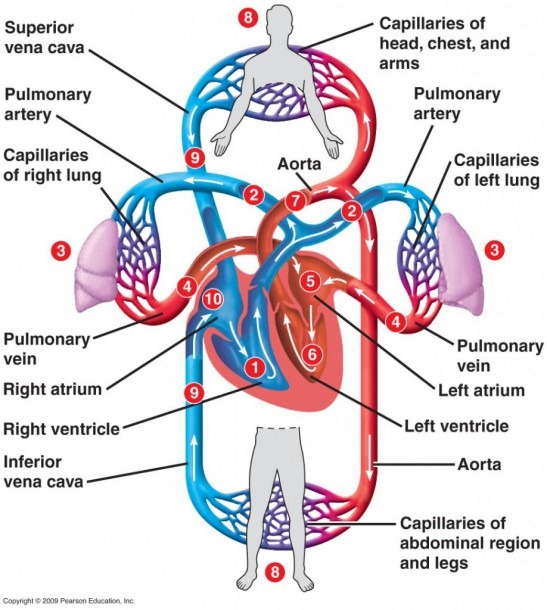
A recent article in JACC discusses inflammatory mediators activated by acute HF and acute kidney injury that can cause both kidney and cardiac injury. More current studies indicate yet another level of interaction between the heart and kidneys. Chronic renal insufficiency can ultimately result in a uremic cardiomyopathy. At the same time, aldosterone and angiotensin can promote myocardial fibrosis by activating galactin III and other inflammatory mediators. 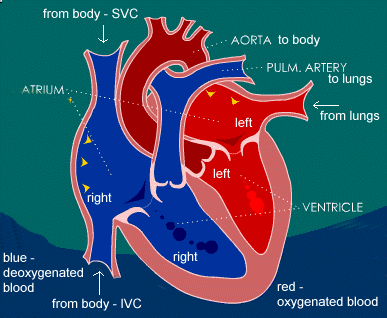
In addition to the hemodynamic problem, inflammatory mediators resulting from acute heart failure also produce kidney injury. The emergence of drugs that increase activity of neuropeptides promises to add an important third leg to HF therapy.Ĭardiac effects on renal function often involve reduction in renal blood flow, venous congestion, and kidney injury related to acute HF. Therapy of HF is based on inhibiting the RAAS and the SNS, and more recently, by augmenting the neuropeptide system that counters effects of the RAAS and the SNS. Heart failure is the best example of these bidirectional regulatory systems gone awry. For example, this occurs with water immersion, causing the well-known phenomenon called swimmer’s diuresis.Īll of these regulatory systems are focused on maintaining normal blood volume, normal blood pressure, and normal tissue perfusion. The atria can be stretched by shifts of blood from the venous system into the central circulation. The natriuretic peptides stimulate the kidney to excrete more water and attempt to restore blood volume to normal. The most relevant is the release of natriuretic peptides from cardiac tissue when the atria are stretched from excess blood volume. The heart also has regulatory effects on the kidney. It is apparent that many of our therapies for cardiac disorders are targeted to the kidneys. SNS stimulation in HF similarly results in toxic effects on the myocardium. So the efforts of the kidney to preserve renal blood flow and filtration actually become detrimental in HF, and RAAS inhibition is an important goal of therapy. Overactivity of the RAAS becomes detrimental to the heart, both by maintaining a high afterload and stimulating sodium and water retention, and by direct toxic effects of angiotensin on the myocardium. When cardiac output is reduced due to impaired left ventricular function, the kidneys again release renin in an attempt to increase blood pressure and preserve renal blood flow. We must pay close attention to the RAAS and SNS in heart failure (HF). The reduction in sympathetic nervous system (SNS) activity also seems to have a positive effect on atrial and ventricular arrhythmias. Additionally, we now understand that the kidney controls sympathetic activation, and ablation of the sympathetic nerves to the kidney can significantly affect blood pressure. 
Blocking the angiotensin receptor site with a receptor blocker also stands as an important component of hypertension management. 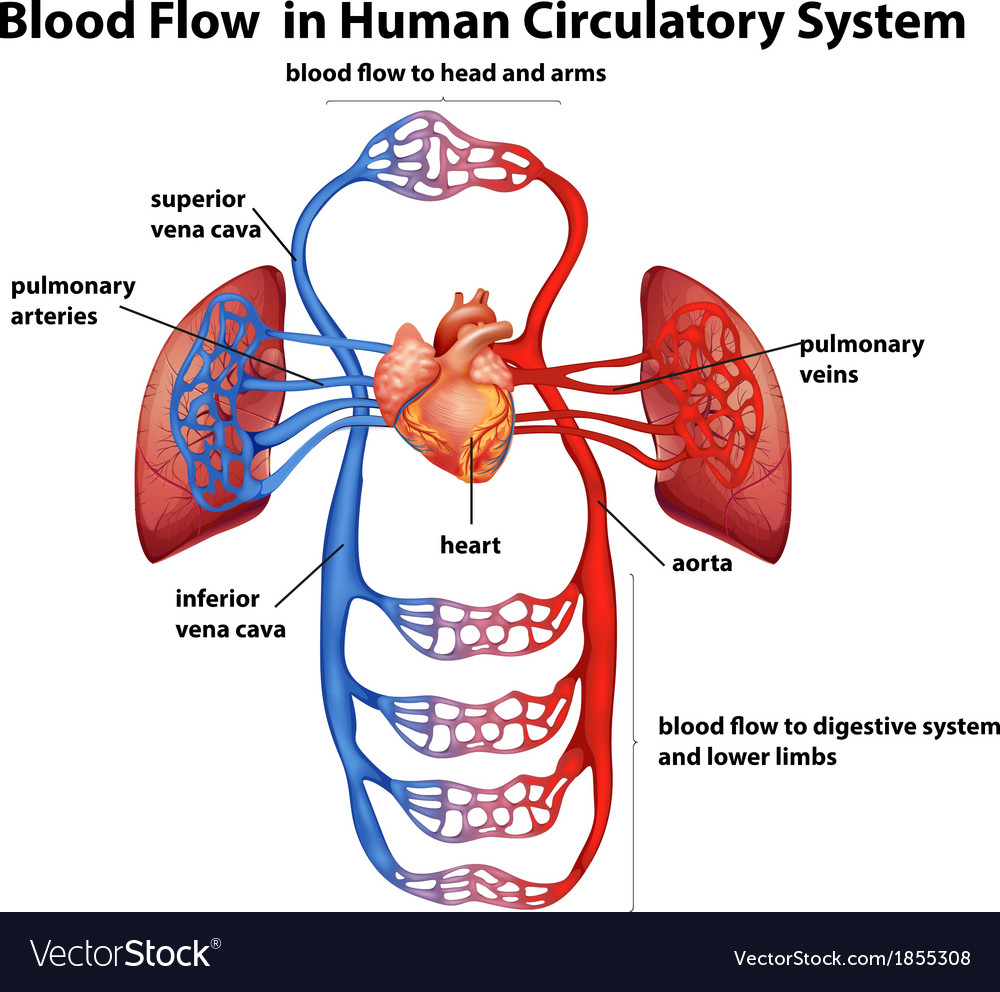
The renin-angiotensin-aldosterone system (RAAS) has become an important component of hypertension management where inhibition of angiotensin activation by an angiotensin-converting enzyme inhibitor has become a mainstay of hypertension management. This again is a system built into the kidney to preserve blood flow, so if the renal blood flow drops, release of renin increases blood pressure to restore blood flow to normal.Īngiotensin also stimulates release of aldosterone that results in sodium and fluid retention to expand blood volume. We also learned that the kidney boasts important blood pressure regulatory functions. He developed the clearance method of measuring glomerular blood flow and described the blood flow control that the kidney exerts to maintain a constant filtration pressure. All of this goes back to our early understanding of renal blood flow, which can be attributed to the physiologist Homer Smith, MD. This month’s cover story reviews the latest information on how the cross-talk between the heart and kidneys should be taken into account when we’re considering pharmacologic or interventional therapy. As we learned in physiology class, the kidney incorporates intrinsic regulatory systems to maintain a constant blood flow to allow appropriate filtering of plasma for excretion of urea and maintenance of fluid volume and sodium balance. We have known for many years that the kidney is more than a filtration organ tasked with removing waste and maintaining volume homeostasis. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
